


Full 1
Full 1
Full 1
Introduction:
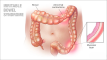
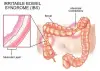
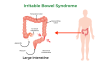
Irritable Bowel Syndrome (IBS) is a common functional gastrointestinal disorder that affects the large intestine (colon). It is characterized by a group of symptoms, including abdominal pain or discomfort, bloating, and changes in bowel habits, such as diarrhea, constipation, or alternating between the two.
The exact cause of IBS is not fully understood, but it is believed to result from a combination of factors, including:
1. Abnormal gut motility: People with IBS may experience abnormal contractions of the muscles in the intestines, leading to changes in bowel habits.
2. Visceral hypersensitivity: Individuals with IBS may have a heightened sensitivity to pain and discomfort in the intestines.
3. Abnormal gut-brain interaction: The communication between the gut and the brain may be altered in people with IBS, leading to exaggerated responses to normal digestive processes.
4. Inflammation and changes in gut microbiota: Some studies suggest that inflammation and imbalances in the gut microbiota may play a role in IBS, but the exact mechanisms are still being studied.
2. Visceral hypersensitivity: Individuals with IBS may have a heightened sensitivity to pain and discomfort in the intestines.
3. Abnormal gut-brain interaction: The communication between the gut and the brain may be altered in people with IBS, leading to exaggerated responses to normal digestive processes.
4. Inflammation and changes in gut microbiota: Some studies suggest that inflammation and imbalances in the gut microbiota may play a role in IBS, but the exact mechanisms are still being studied.
IBS is a chronic condition, and its symptoms can be triggered or exacerbated by various factors, including certain foods, stress, hormonal changes, and infections. It’s essential to note that IBS does not cause permanent damage to the intestines or increase the risk of developing serious conditions like colorectal cancer.
The primary symptoms of IBS include:
- Abdominal pain and cramping: Often relieved after a bowel movement.
- Bloating: A feeling of fullness and distention in the abdomen.
- Changes in bowel habits: Alternating between diarrhea and constipation, or experiencing one more frequently than the other.
- Mucus in the stool: Some people with IBS may notice mucus in their bowel movements.
- Urgency: A sudden and intense need to have a bowel movement.
Diagnosis of IBS is typically based on the patient’s symptoms and the absence of other significant gastrointestinal disorders. However, healthcare providers may order tests to rule out other conditions with similar symptoms.
The management of IBS aims to alleviate symptoms and improve the individual's quality of life. Treatment options include:
- Lifestyle modifications: Making dietary changes, managing stress, and incorporating regular exercise can help manage IBS symptoms.
- Medications: Over-the-counter options, such as antispasmodics and laxatives, may provide relief for some people. In more severe cases, prescription medications like antidepressants, antidiarrheals, or medications targeting gut motility may be prescribed.
- Cognitive-behavioral therapy (CBT): CBT can help individuals cope with stress and manage symptoms.
- Probiotics: Some individuals find relief from certain probiotics that help balance the gut microbiota.
- FODMAP diet: Some people with IBS may benefit from following a low-FODMAP diet, which involves avoiding specific fermentable carbohydrates that can trigger symptoms.
It’s essential for individuals with suspected IBS to seek medical evaluation and guidance. A healthcare provider can provide an accurate diagnosis and develop a personalized treatment plan based on the individual’s symptoms and needs.
