


Full 1

Full 1
Full 1

Introduction:
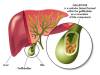
Gallstones are small, solid particles that form in the gallbladder, a small organ located beneath the liver. The gallbladder stores bile, a digestive fluid produced by the liver that helps break down fats in the small intestine during the digestion process.
Gallstones can vary in size and composition, and they are classified into two main types:
1. Cholesterol stones: These are the most common type of gallstones and are formed when there is an excess of cholesterol in the bile. Cholesterol stones are usually yellow-green in color.
2. Pigment stones: These are less common and are formed when there is an excess of bilirubin (a pigment produced from the breakdown of red blood cells) in the bile. Pigment stones are typically smaller and darker in color.
2. Pigment stones: These are less common and are formed when there is an excess of bilirubin (a pigment produced from the breakdown of red blood cells) in the bile. Pigment stones are typically smaller and darker in color.
The exact cause of gallstones formation is not always clear, but some risk factors and conditions that contribute to their development include:
1. Gender: Women are more likely to develop gallstones than men, particularly during pregnancy or when using hormonal birth control.
2. Age: Gallstones become more prevalent as people age, especially those over the age of 60.
3. Obesity: Being overweight or obese increases the risk of gallstones formation.
4. Rapid weight loss: Crash diets or other methods of losing weight too quickly can trigger the formation of gallstones.
5. Diet: A diet high in fat and cholesterol and low in fiber may contribute to gallstone development.
6. Genetics: A family history of gallstones can increase an individual’s risk.
7. Certain medical conditions: Conditions like diabetes, liver disease, and certain blood disorders can increase the risk of gallstone formation.
2. Age: Gallstones become more prevalent as people age, especially those over the age of 60.
3. Obesity: Being overweight or obese increases the risk of gallstones formation.
4. Rapid weight loss: Crash diets or other methods of losing weight too quickly can trigger the formation of gallstones.
5. Diet: A diet high in fat and cholesterol and low in fiber may contribute to gallstone development.
6. Genetics: A family history of gallstones can increase an individual’s risk.
7. Certain medical conditions: Conditions like diabetes, liver disease, and certain blood disorders can increase the risk of gallstone formation.
Diagnosis is typically made through a combination of medical history, physical examination, and tests such as endoscopy, where a flexible tube with a camera is inserted into the digestive tract to visualize the ulcers.
Treatment for peptic ulcers depends on the underlying cause:
1. H. pylori infection: Antibiotics are prescribed to eradicate the bacteria. Acid-suppressing medications like proton pump inhibitors (PPIs) and histamine-2 (H2) blockers are also used to reduce stomach acid production and allow the ulcers to heal.
2. NSAID-related ulcers: Discontinuing or reducing NSAID use is advised. In some cases, alternative pain management options may be recommended.
3. Lifestyle changes: Quitting smoking, avoiding excessive alcohol consumption, and managing stress can aid in the healing process.
2. NSAID-related ulcers: Discontinuing or reducing NSAID use is advised. In some cases, alternative pain management options may be recommended.
3. Lifestyle changes: Quitting smoking, avoiding excessive alcohol consumption, and managing stress can aid in the healing process.
Most people with gallstones do not experience symptoms and may not require treatment. These are called “silent gallstones.” However, if a gallstone becomes lodged in a duct, it can lead to complications and cause symptoms such as:
- Biliary colic: Intense pain in the upper abdomen or right side, which may radiate to the back or right shoulder blade.
- Nausea and vomiting: Due to the blockage of the bile duct.
- Jaundice: Yellowing of the skin and eyes if the stone blocks the bile duct completely.
- Inflammation or infection: If a gallstone causes inflammation of the gallbladder (cholecystitis) or the bile duct (cholangitis).
Treatment for gallstones depends on whether they are causing symptoms or complications. In many cases, surgery to remove the gallbladder (cholecystectomy) is recommended, and it is often performed laparoscopically, resulting in smaller incisions and faster recovery times. Removal of the gallbladder does not typically cause any long-term health problems since the body can still digest fats without it.
If you suspect you have gallstones or are experiencing any symptoms related to gallbladder issues, it’s essential to seek medical advice from a healthcare professional. They can provide an accurate diagnosis and recommend the appropriate treatment plan.
